By now, you’ve likely heard the news that a low-fat diet is no good. Learn why grass fed is better when choosing your healthy fats and how to eat the ideal ratio of omega 3 to 6 fats.
Omega-3 fats are getting a lot of attention these days, but they’re not a panacea. No miracle cure exists for what ails us. Nonetheless, omega-3s do have a unique place in the evolving discussion of which foods to eat. Think of omega-3s as a gateway fat — a portal into a bigger, fuller, richer story of fats in general.
Fats are complicated, a fact we must embrace. It was, after all, an oversimplification that persuaded experts to recommend avoiding them for the past 40 years. Consider, for example, how the popular mantra “You get fat because you eat fat” relates to a cornerstone of contemporary medicine: “Cholesterol in our blood derives from eating certain fats, and causes the heart disease that kills us.”
None of this is true. Despite prominent critiques over the past decade by writers such as Mary Enig, Ph.D., Gary Taubes, and Nina Teicholz, these anti-fat articles of faith spawned legions of unctuous fat nags, cholesterol screenings, skin-trimmed chicken breasts, Egg Beaters, and margarine. All of this was wrong, yet, until recently, the medical industry has stuck by its low-fat guns.
Article at a glance:
• Fats in Your Kitchen
• Small Changes, Big Results: Dietary Changes to Improve Omega-6 to Omega-3 Ratio
How Bad Advice Brought Bad Health
The long-recommended health guidelines that demonized all fat ultimately increased the amount of recommended carbohydrates in our diets. Unlike fats, carbohydrates are simple. Some carbohydrates are called “complex” — such as whole-wheat flour and potato starch — but all carbohydrates eventually reduce to sugars, which then reduce to glycogen. An overload of carbohydrates triggers an insulin response, leading eventually to insulin resistance — one of the markers associated with metabolic syndrome, which underpins obesity, diabetes, heart disease and the related inflammation.
Our bodies run on combustion, so we eat carbohydrates with the belief that glycogen is the fuel of life — but fat is fuel, too. Fats burn just fine. They just don’t reduce to a single, simple molecule. Your body will use fats in all of their rich variety — monounsaturated, polyunsaturated and saturated.
Fats perform many tasks in your body: They provide energy, wire brain neurons, allow bones to absorb calcium, prevent blood clots, mediate inflammation, and speed nervous-system response — to name a few. At the same time, fats provide the medium for a whole array of micronutrients to perform their specialized jobs; that is, fats assist in bioavailability.
For example, a person short on one simple vitamin or nutrient often can’t correct the deficiency by taking a vitamin supplement. If the other components of basic transport and chemical reactions aren’t present to allow the body to use that vitamin, that person won’t absorb its benefits. Fats enable bioavailability for a variety of nutrients, including carotenoids and the fat-soluble vitamins A, D, E and K.
On some fat-related issues, mainstream consensus has emerged on what is actually good versus bad. Trans fats, for instance, are now understood to be the original Frankenfood. Trans fats derive their name from a simple transposition in molecular structure, a rejiggering that creates a molecular geometry without evolutionary precedent. While some trans fats are naturally occurring, artificial trans fats are found in industrially processed, hydrogenated vegetable oils. Whipped up as a cheaper alternative to lard in the early 20th century, artificial trans fats are the core of shortening and margarine; both are thinly disguised vegetable oils previously touted as healthful substitutes for allegedly harmful animal fats.
Many biochemical processes in your body work by pairing shapes of molecules to receptors, like keys fitting into locks. When your body doesn’t recognize a molecular shape, it treats the stranger as an invader, and fights it with the immune response of inflammation. Trans fats have an unrecognizable shape, which is why the U.S. Food and Drug Administration now officially lists trans fats as unsafe to eat. Yet they remain the lubricant in much of fast and processed food.
An advisory committee that guides federal nutrition policy signaled an even bigger shift in February 2015 by reversing long-standing advice to avoid foods high in saturated fats, such as butter and lard, and those high in cholesterol, such as eggs.
Omega-3s and Omega-6s
Many of the fats labeled “essential fatty acids” perform particular, unique, and, yes, essential tasks to keep our bodies running. These fatty acids have no substitutes, and for the most part can’t be made within our bodies. The litany of essential fats is a daunting string of polysyllabic nomenclature only a chemist could love, and you can’t boil it down. Our health and intelligence depend on filling every gap on the list.
Here’s where omega-3s enter the story: The damage wrought by removing them from our bodies is easy to spot, well-researched and frightening. A lack of a particular omega-3 — docosahexaenoic acid, or DHA — undermines the function of our brains. As the British journalist Graham Rose famously wrote, we are in danger of creating “a race of morons” because of the omega-3 deficiency in contemporary diets.
The research is clear.
Here’s the scary news: Most of us eating modern diets aren’t getting enough of these crucial omega-3 fats.
Omega-3 is not the name of a single kind of fat molecule, but rather is an umbrella term for a set of five similar fat molecules.
Like omega-3, omega-6 is an umbrella term for a number of fatty acids, and the key one is linoleic acid. Linoleic acid is the primary fat in corn, soy, cottonseed, safflower and sunflower oils. Modern industrial agriculture and food processing have replaced the DHA we once consumed with linoleic acids from vegetable oils. As shown in this chart of the omega-3 and omega-6 content of various cooking oils, your choice of cooking fat matters. On average, since the late 1960s, U.S. diets have risen from 1 percent linoleic acids to 8 percent because of direct consumption of these oils coupled with indirect consumption via factory-farmed meat, eggs, dairy and fish.
A growing number of researchers focus on one specific omega-3 fatty acid, DHA. This unique essential fat is fundamentally important to humans and all life, and it is critical to brain function. A shortage of DHA is linked to a wide range of brain malfunctions, including:
- Attention-deficit disorder
- Dementia
- Depression
- Low IQ
- Manic depression
- Memory loss
- Schizophrenia
- Violent behavior
The brain runs on fat, but this is not a brain issue alone.
The prevailing advice, to choose vegetable oils rather than animal fats, may also have raised obesity rates by lowering DHA concentrations in red blood cells. It’s important to realize that while other omega-3s have particular functions, they can’t substitute for DHA. Eating more omega-3s will not stave off these problems unless an adequate amount of DHA is in the mix.
For instance, omega-3 alpha linolenic acid (distinct from omega-6 linoleic acid), the omega-3 found mostly in plants, is the precursor of DHA (hence the “alpha”). Your body can convert alpha linolenic acid to DHA, but only in a slow and inadequate manner.
The best contemporary source of DHA is cold-water fish, such as salmon and tuna. Can we solve these urgent health problems simply by eating more fish? J.T. Winkler, a British researcher of nutrition policy, provided a blunt answer to another key question: “Are there enough fish in the sea to provide the amounts we need? No.” It seems our species has overpopulated its habitat to the point of severe malnutrition, in addition to the significant harm we’ve done to other species.
The industrial solution to overfishing seems to be aquaculture, or farmed fish. But that “solution” is a dead end, and the reason is illuminated by the term some apply to farmed fish: “floating vegetables.” Farmed fish would ideally get omega-3s mostly by eating fish meal and fish oils, but they don’t. Farmed fish become “floating vegetables” simply because aquaculture worldwide feeds vegetable oils to farmed fish, a practice that has left them with an unnatural and unhealthful omega-6 to omega-3 ratio — the same defect of all factory-farmed foods.

The problem is that foods high in omega-6 — notably soy and corn oils, as well as factory-farmed meat and dairy — produce such a surplus of omega-6 fatty acids that the beneficial omega-3 fats can’t compete. When omega-6s flood your system, they use up all the molecular sockets needed by omega-3s, so the latter are blocked from doing their jobs. The modern U.S. diet has an omega-6 to omega-3 ratio of more than 10 to 1. Research shows we evolved with a ratio closer to 1 to 1, and would be a lot healthier if we could achieve that again.
A Norwegian researcher looking at diets fed to farmed fish and lab animals found that the simple switch in concentrations of these two key fatty acids to favor omega-6s provoked obesity and inflammation. Restoring the ratio to a more natural balance reversed both obesity and inflammation.
Eat Less Omega-6 and More Omega-3
Because of the ubiquitous use of high-omega-6 corn and soy to feed livestock and produce cheap, processed foods, the average contemporary diet is four times higher in omega-6 fatty acids than it should be for optimal health. This elevated level of omega-6 intake interferes with the essential functions of omega-3 fatty acids. For ideas on how to modify your diet to improve your ratio, see our chart on a sample daily intake.
Current omega-6 to omega-3 ratio in the Standard American Diet: 15 to 1*
Optimal omega-6 to omega-3 ratio: 4 (or lower) to 1**
Recommended omega-3 consumption with elevated omega-6: 3,600 mg/day**
Recommended omega-3 consumption with reduced omega-6: 360 mg/day**
*Source: USDA
**Source: Dr. Joseph Hibbeln, NIH
Finding the Real Solution: Sources of Healthful Fats
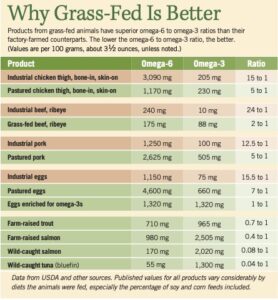
Oddly, studies of omega-3 sources have focused almost exclusively on fish, and were this the end of the story, humanity would be in a terrible jam. Red meat from beef and pork, as well as poultry meat, has been generally ignored, simply because grain-fed animals face exactly the same problem as farmed fish: They’re fed corn and soy, which are so high in the wrong kind of fats. Almost all the beef, pork and poultry raised in the United States comes from animals fed such a diet, which is cheap in more ways than one, and fattens them up quickly. Their meat, milk and eggs are significantly different from products that come from animals raised on their original, pastured diets. (Grass-fed is better chart.)
As is the case with wild fish, products provided by pasture-raised animals deliver the DHA we require. While grass-fed beef, eggs and dairy products are not as rich in DHA, pound for pound, as wild, cold-water fish, they still have it in abundance.
Besides DHA, there are four other discrete omega-3s, and each has a role to play. Compared with feedlot products, milk and meat from pasture-raised animals also have 300 to 500 percent more conjugated linoleic acid, or CLA — another omega-3 fatty acid (distinct from omega-6 linoleic acid). This CLA offers benefits for brain health different from those of DHA. In addition to linoleic acid, there are three other omega-6s, each with vital functions, especially in our immune systems — and this only accounts for two groups of the polyunsaturated fats.
Taken together, all of this evidence drives a “steak” in the heart of fat-phobic advice and warnings about high cholesterol. The widespread and unanimous evidence correlates reduced omega-3 fats with reduced brain function, especially the long-term, corrosive effects that lead to dementia and Alzheimer’s disease. Research even shows a connection between the widely prescribed statin drugs that lower blood cholesterol, such as Lipitor, and reduced brain function. This is not a side effect of the drugs, but a primary effect — statins reduce cholesterol. Now, consider that while your brain is about 2 percent of your body’s weight, it holds about 25 percent of your body’s cholesterol, and is composed of approximately 60 percent fat. In short, your brain must have cholesterol.
All of this is widely variable depending not just on food source, but also on season, storage conditions, integrity of suppliers, and the perishability of some of these fats. There are no guarantees, but this story hangs together: The complexity itself is what we need to seek, not just this fat or that wonder micronutrient.
The following, simple rules will point us in the right direction:
- Avoid processed foods. They’re loaded with soy- and corn-based ingredients, and are too high in sugars, as well as preservatives and other dubious additives.
- Embrace variability. Don’t take all of your eggs out of one basket. Seek rich sources of omega-3s, especially DHA, and the rest of the essential fatty acids will come with the package.
- Don’t rely on supplements. Even the best have serious drawbacks with perishability and bioavailability. At its worst, the industry is riddled with snake oil and fraud.
- Choose wisely and eat well. The best sources of healthful fats and the whole array of micronutrients are wild, cold-water fish; wild game; and meat, dairy and eggs from grass-fed animals. Complement those with the abundant micronutrients and fats in fresh, unprocessed foods, nuts, fruits and vegetables — and see what you think. Or, more accurately, see how you think, and how you move and feel.
Read more about this topic in The Big Fat Lies and on the Essential Fatty Acids Education website, a website maintained by scientists at the National Institutes of Health. — MOTHER
Richard Manning is the author of Against the Grain: How Agriculture Has Hijacked Civilization, and, with Dr. John Ratey, of Go Wild.







